As many as 15% of women aged 15 to 50 are thought to have polycystic ovarian disease (PCOS). While the condition can cause distressing symptoms, it can also affect your reproductive health and may increase your risk of developing other chronic health problems. However, a range of treatments are available for PCOS, which can help to manage your symptoms and make complications less likely. Assessment and diagnosis of your symptoms by an experienced gynaecologist with a specialist interest in polycystic ovaries is therefore essential to help you start the right treatment promptly.
You are most likely to develop signs of polycystic ovarian disease between puberty and your mid-twenties. Even though not every woman develops the full range of symptoms associated with this condition, you are most likely to experience the following:
1/ Irregular periods, which may stop for months at a time
2/ Weight gain or difficulty losing weight, but women with a healthy or low body weight can also develop PCOS
3/ Noticeable hair growth on your face, chest, stomach and back, though you might find that you experience hair loss from your scalp as well
4/ Acne
5/ If you are trying for a baby, you may find that you struggle to conceive
With a combination of these symptoms, you should always seek medical advice, as tests can show whether you have PCOS or another condition.
Although it is not exactly clear what causes polycystic ovaries, women with PCOS often have insulin resistance, which means your body doesn't respond to the action of the hormone as it should. Insulin resistance also occurs in type 2 diabetes and causes high blood sugar levels, though in PCOS it leads to increased production of the male hormone testosterone. High levels of testosterone are responsible for symptoms such as hair growth and acne, as well as affecting your menstrual cycle. Your periods become irregular or stop in polycystic ovarian disease.Your ovaries develop tiny cysts, which prevents the regular release of an egg each month.
Even though polycystic ovaries are not dangerous and do not make you more susceptible to ovarian cancer, getting diagnosed earlier offers you symptom relief and can help to restore your fertility and prevent some gynaecological problem like cancer of the lining of the womb. Prompt diagnosis may also help to protect you from type 2 diabetes and cardiovascular disease, which are more likely when you have insulin resistance.
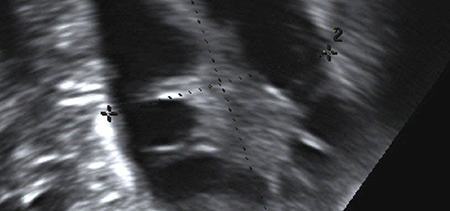
Besides assessing your symptoms, it is usual to check your blood levels of female and male sex hormones, as well as carrying out an ultrasound scan of your ovaries. However, other blood tests may also be necessary to exclude another condition such as an underactive thyroid or Cushing's disease. Current guidelines for PCOS diagnosis are that having two or more out of the three following confirms you have the condition:
1/ The presence of polycystic ovaries on an ultrasound scan
2/ Irregular or absent periods
3/ Signs of raised testosterone, either from the results of blood tests or from your symptoms
Although these guidelines are in place, choosing an experienced gynaecologist makes sure that you receive the correct diagnosis and treatment.
Although medical and surgical options are available for the management of polycystic ovarian disease, lifestyle changes also play an important role. Weight loss and exercise both reduce insulin resistance, which in turn increases your chances of ovulation and successful pregnancy, as well as reducing your risk of diabetes and heart disease. However, even if you are not overweight, following a low glycaemic index diet can help to stabilise your blood sugars, leading to improved symptoms and health.
The additional treatment you receive will be tailored to your individual needs. For instance, if you are not planning a pregnancy, combined oral contraceptives can aid menstrual regularity, while Metformin can reduce insulin resistance and improve your symptoms. Metformin is also known to improve your chances of pregnancy, but you may also need Clomifene to trigger ovulation. However, Metformin has some side effects like abdominal cramps and bloated-ness and recently another medicine called Inofolic has come in use. This is a dietetic supplement and is vegetable origin, free of gluten and lactose. Insulin-resistance is a significant feature in women with PCOS and Clinical trials have shown that Inofolic supplementation increases the insulin sensitivity by 84%. Researches have shown that it helps with weight loss in conjunction with ultra-low carbohydrate diet. It produces ovulation in majority of women with anovulation due to PCOS.
Dr Sheela Purkayastha will use her expertise in PCOS to carefully decide on the most suitable treatment for you. If you would like to make an appointment with Dr Purkayastha, call now to arrange a consultation for specialist advice.

![]() Privacy Policy | Disclaimer | Links | Sitemap | View Mobile Website
Privacy Policy | Disclaimer | Links | Sitemap | View Mobile Website
The contents on this site is for information only, and is not meant to substitute the advice of your own physician or other medical professional.